Your Date With Brain Destiny
Can you believe that I have been so bold as to claim that lifestyle factors, over which we have control, may play a role in determining whether or not we develop Alzheimer’s disease? To be sure, I read the criticism from the skeptics and have elected not to fan the flames by commenting on their blog sites. There are those who cling to the idea that what we eat, how much exercise we get, whether we sleep enough and even whether we put ourselves in stressful situations matters little in terms of the fate of our brain function.
This ideology is flawed on at least two counts. First, it relinquishes your cognitive fate to a prescription for an as of yet nonexistent drug. Second, it is not in line with our most current and well-respected scientific journals. Nonetheless, some people tend to be “down on what they are not up on.”
Let’s take a look at what our thought leaders are telling us. Dr. Deborah Barnes is a neuroscientist in San Francisco. Her work gets published in some of our most highly regarded journals. She recently published some really great science in Lancet Neurology in which she concluded that factors like obesity, diabetes and high blood pressure dramatically increase a person’s risk for developing Alzheimer’s disease.
As reported by the University of California, San Francisco:
Over half of all Alzheimer’s disease cases could potentially be prevented through lifestyle changes and treatment or prevention of chronic medical conditions, according to a study led by Deborah Barnes, PhD, a mental health researcher at the San Francisco VA Medical Center (SFVAMC). Analyzing data from studies around the world involving hundreds of thousands of participants, Barnes concluded that worldwide, the biggest modifiable risk factors for Alzheimer’s disease are, in descending order of magnitude, low education, smoking, physical inactivity, depression, mid-life hypertension, diabetes and mid-life obesity.
In the United States, Barnes found that the biggest modifiable risk factors are physical inactivity, depression, smoking, mid-life hypertension, mid-life obesity, low education and diabetes. Together, these risk factors are associated with up to 51 percent of Alzheimer’s cases worldwide (17.2 million cases) and up to 54 percent of Alzheimer’s cases in the United States (2.9 million cases), according to Barnes.
This is powerfully important information. Fifty-four percent of Alzheimer’s patients in America didn’t have to get this devastating diagnosis – if they had only known. Yet, somehow we are supposed to buy into the notion that we can live our lives however we choose and that soon there will be a cure for whatever malady befalls us.
As of this writing, there is no meaningful treatment for Alzheimer’s disease. Several months ago, to great fanfare, federal monies, to the tune of $33 million, were allocated to help pharmaceuticals develop a drug to prevent Alzheimer’s, a disease affecting more than 5.4 million Americans.
In my commentary on MindBodyGreen I wrote:
While the idea of creating a drug to prevent Alzheimer’s seems honorable, it’s important to consider that the development of such a drug means big business beyond measure. Deutsche Bank estimates that the development of an efficacious drug treatment for the disease once it has taken hold could generate $20 billion in annual sales. But the value of a drug employed to treat people before there is any evidence of dementia—a far larger treatment group compared to those already afflicted—would be staggering.
New York Times writer Pam Belluck reported that the goal of this grant would be to develop a preventive treatment using a strategy much like the one for heart disease. Belluck quoted Laurie Ryan, program director for the Alzheimer’s clinical trials at the National Institute on Aging, who said, “We’re going to look at people at risk, just like we do with people who have high cholesterol and are at risk for cardiovascular disease.
Is this really what we should be doing? We already know that modifiable lifestyle factors profoundly influence Alzheimer’s risk, but, as I recently wrote for The Daily Beast:
The fundamental operating system underlying the practice of medicine in America today seems myopically focused on treating our ills with highly profitable remedies directed at symptom management while causality is ignored. Preventing disease is derogated, and relegated to the province of alternative modalities. Watching our elected leaders debate the merits of funding the ever-changing iterations of a health-care plan designed to treat illnesses presents a poignant irony, as it has little to do with health and everything to do with illness. But it has become clear that both sides of the aisle enthusiastically agree that Americans must have access to their pills, and lots of them.
Just the simple act of getting regular exercise can dramatically lower Alzheimer’s risk, and this isn’t new information. In fact, exercising regularly has been demonstrated to actually improve memory in adults with memory impairment. Where would such an iconoclastic report have been published? It was published in the Journal of the American Medical Association way back in 2008!
So it’s time we accept the idea, with gratitude, that from a cognitive perspective, how we live our lives matters a whole lot in determining how we will be functioning in the future. Dietary choices determine blood sugar levels and even mild elevation of blood sugar levels translates to a dramatically increased risk for dementia, as recently reported in The New England Journal of Medicine. Keep in mind that this study showed a marked increased risk for dementia even in individuals without diabetes or even pre-diabetes.
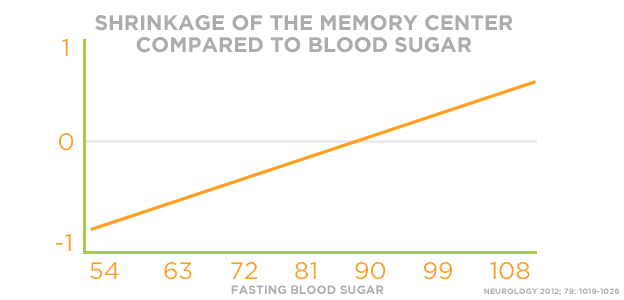
In fact, there is a direct relationship between fasting blood sugar and the rate of shrinkage of the hippocampus (the brain’s memory center), as demonstrated in a recent issue of the state of the art journal Neurology. When it comes to your brain’s memory center, size does matter.
As the authors of this study stated in their conclusion:
High plasma glucose levels within the normal range were associated with greater atrophy of structures relevant to aging and neurodegenerative processes, the hippocampus and amygdala. These findings suggest that even in the subclinical range and in the absence of diabetes, monitoring and management of plasma glucose levels could have an impact on cerebral health.
And what should your first step be in terms of “management of plasma glucose?” To dramatically reduce carbohydrate intake while increasing your consumption of healthful fats. This is a central theme of the Grain Brain program and is fundamentally supported by a recent publication by researchers at the Mayo Clinic in the Journal of Alzheimer’s Disease. They found that elderly individuals favoring a high carbohydrate diet experienced an increased risk for developing dementia of close to 90% while the dementia risk was decreased by 42% in those consuming the most fat.
I encourage you all to read these citations and embrace the empowerment that this knowledge provides in terms of changing your brain’s destiny.
For more information, order your copy of Grain Brain today and join Dr. Perlmutter’s email list.













